Funded by the Canadian Frailty Network 2014-2016 (Formerly TVN)
Project Overview
Residents living and dying in long-term care (LTC) homes represent one of society’s most frail and marginalized populations of older adults. The main goal of this research project was to adapt, implement, and evaluate a multi-component palliative care program, called Strengthening a Palliative Approach in Long Term Care (SPA-LTC). The project used a multiple case study design and participatory action approach in collaboration with four LTC homes in southern Ontario.
Click here for more information about the Strengthening a Palliative Approach in Long-Term Care (SPA-LTC) ProjectClick here for information on the SPA-LTC Model
Resources
Research Brief Handouts
Click on the images below to download the pamphlets in PDF file formats
- A Stakeholder Analysis of the Strengthening a Palliative Approach in Long Term Care (SPA-LTC) Model
- An Analysis of Documents Guiding Palliative Care in Five Canadian Provinces
- End-of-Life Care and Resident Comfort in LTC: Perceptions of Bereaved Caregivers
- The Strengthening a Palliative Approach in Long-Term Care (SPA-LTC)
Program: An Evaluation - “Now I don’t have to guess”: Using Pamphlets to encourage residents and
families/friends to engage in advance care planning in long-term care - What are the differences among occupational groups related to their
palliative care-specific educational needs and intensity of interprofessional
collaboration in long-term care homes? - Exploring the End-of-Life Care and Bereavement Needs of Family Members
in Long-Term Care Homes - “Who would want to die like that?”: Perspectives on Dying Alone
- Meaningful connections in dementia end of life care in long term care homes
- Mind the gap: Is the Canadian long—term care workforce ready for a
palliative care mandate? - Heart work: A thematic analysis of compassion in long-term care
- Whose role is it anyways? Using pamphlets to activate early conversations
about end-of-life care in long-term care - Family Care Conferences in Long-Term Care: Exploring Content and
Processes in End-of-life Communication - Broadening End-of-Life Comfort to Improve Palliative Care Practices in
Long-Term Care
The Impact of Illness Trajectory Pamphlets
Ontario Specific Pamphlets
Click on the images below to download the pamphlets in PDF file formats.
Alberta Specific Pamphlets
Click on the images below to download the pamphlets in PDF file formats.


Alberta Advanced Kidney Failure, Frailty & Dementia Pamphlets – Coming Soon!
Saskatchewan Specific Pamphlets
Click on the images below to download the pamphlets in PDF file formats.


Saskatchewan Advanced Kidney Failure, Frailty & Dementia Pamphlets – Coming Soon!
Manitoba Specific Pamphlets
Click on the images below to download the pamphlets in PDF file formats


Manitoba Advanced Kidney Failure, Frailty & Dementia Pamphlets – Coming Soon!
As a part of the Strengthening a Palliative Approach in Long-Term Care (SPA-LTC) Study, five educational illness trajectory pamphlets were developed. The pamphlets focus on five life-limiting chronic illnesses that are most prevalent and inadequately addressed in LTC; frailty, dementia, heart failure, kidney disease, and lung disease. The pamphlets aim to provide information to residents and family about the expectations of each illness, prompting questions from family and availability of resources from LTC. Along with providing information, the pamphlets aid in activating Advance Care Planning (ACP); the process of discussing values and wishes about future care for the resident between residents, families, and staff. Advance care planning typically has many barriers in LTC, including staff discomfort, lack of initiative and reluctance from family members, and lack of available tools to support such discussions. The pamphlets provide a tool to initiate the discussion of end-of-life care and activate Advance Care Planning.
The Strengthening a Palliative Approach in Long-Term Care Palliative Care Model
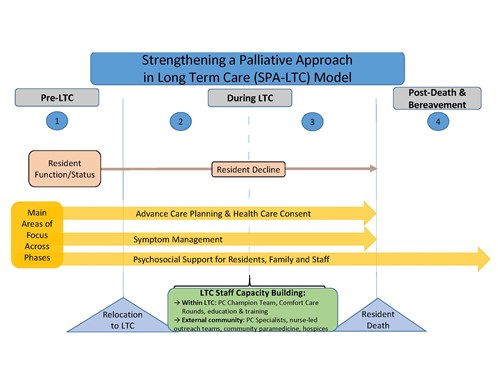
The Strengthening a Palliative Approach in Long-Term Care Palliative Care Model includes four Phases: (a) Before Entering LTC, (b) After Moving in to LTC, (c) Progressing into Advanced Illness/End of Life, (d) and Grief and Bereavement. It has been developed based on a synthesis of the literature and feedback from key stakeholders, including LTC staff. The core programmatic features include: information and resources for residents and family to support a palliative approach philosophy to care; mechanisms to help staff identify and activate a change in care planning based on key transition points; formalized opportunities for communication between staff, residents and families; team-building strategies, champions teams and collaborative learning opportunities within LTC; and leveraging supports and resources external to the LTC sector.
Key Activities of Each Phase of the SPA-LTC Model
Phase 1. Pre-LTC
- Assess resident needs within a holistic model with attention to existing chronic diseases, frailty
- Ensure adequate support is provided if on waiting list for LTC; avoid crisis admissions
- Allow for fluid movement into LTC and back out if resident condition warrants it
Phase 2. After Relocating to LTC
- Support resident and family during adjustment to living in LTC; address ‘losses’ of resident and family
- Complete full assessment upon admission, including medication review and level of frailty; ongoing as deemed necessary
- Introduce concept of a palliative approach to residents and family & prepare them for expected changes in health conditions
- Begin proactive discussion with resident and family about wishes and values/advance care planning with preferred tools
- Discuss CPR options and develop plan of care at 6-week conference
Significant Resident Decline/Advanced Chronic Illness Triggered By One or More of the Following:
- 2 or more indicators checked on SPICT (Supportive Palliative Care Indicators Tool)
- PPS (Palliative Performance Scale) score <30%
- J5 checked on RAI MDS
- ‘No’ to the question: “Would you be surprised if the resident died within 6 months?”
Phase 3. Advanced
Illness/End of Life
- Support the resident and family through life review, emerging issues, and final separation
- Revisit wishes and values/advance care planning discussions, including preference of place of care; hold Palliative Family Care Conference, identify goals of care & obtain informed consent (see forms); ensure resident/family’s questions are addressed
- Review medications in consultation with the physician, pharmacist and nurse; continue only those deemed necessary or for comfort measures
- Ensure end of life medications are prescribed and dispensed for residents at beginning of this phase, not the end (see medication form)
- Continue to monitor symptoms especially pain, anxiety, dyspnea, constipation
- Help prepare residents and family for changes, especially physical, in last hours of life
Phase 4. Grief & Bereavement
- Provide after death care & guidance for family about funeral arrangements
- Communicate and provide support to other residents
- Acknowledge death, i.e. send sympathy card, hold memorial services
- Provide written material regarding loss, bereavement and available resources
- Offer bereaved family members the opportunity to attend a peer support group
More about the SPA-LTC Project Findings
Baseline
- Focus groups with LTC home staff, residents, and families (N=20) highlighted that understandings of comfort limited the integration of palliative care principles to the final days of residents’ lives
- Support staff’s comfort of working with dying patients and their level of interdisciplinary coordination were significantly lower compared to both nurses and PSWs
- Bereaved family members who perceived a resident as having received good care reported less resident emotional distress at end-of-life and those families who received support from staff perceived less resident emotional distress at end of life
- Chart audits revealed that 26% of LTC residents on average across all four sites died in the past year with the majority of resident deaths occurring at the LTC home; 65.3% of them visited Emergency Departments (ED) during the last year of life; 45.8% with ED visits in last month of life and 27.1% occurred during their last week of life
SPA Implementation and Evaluation
- Palliative Care Champion Teams: Increased interdisciplinary communication and cooperation providing a gateway for staff to access palliative care information and resources
- Comfort Care Rounds (CCRs): Provided monthly opportunities for collective problem-solving and case based learning. Common issues discussed included managing sudden resident deaths, navigating complex family dynamics, and balancing the divergent needs of families and residents.
- Illness Trajectory Pamphlets: Were seen as providing valuable information to residents and families about what to expect with different health conditions. Information about what a palliative approach is and how advance care planning (ACP) can support quality end of life care were particularly appreciated by residents and families. Two-thirds of residents and family members reported increased comfortable exploring ACP after reading a pamphlet.
- Family Care Conferences: were offered to 62% of enrolled residents. Issues most commonly discussed were preferences for physical and care at end-of-life. Conferences that were interdisciplinary discussed more aspects of end-of-life care. The majority of families who participated in the conferences reported their concerns and issues around end of life care were addressed and that the conferences were valuable in supporting good communication with staff.
Outcomes
- There were no significant pre-post differences of bereaved families’ perceptions of residents’ end of life comfort and families’ overall perceptions of care
- Chart audit revealed reductions in the number of ER visits, more planned or appropriate ER visits and fewer ER admissions that became hospital admissions
- Staff’s, resident’s and families’ perceptions of all components of the SPA-LTC intervention were positive and indicated perceived improvements in communication and comfort with end-of-life issues
Impact
The importance of our findings to the care of the seriously ill, frail elderly and their caregivers revealed that with the implementation of this program we can improve advance care planning uptake and end of life communication for those living and dying in LTC and their families, decrease hospital transfers at the end of life and increase satisfaction of care for all stakeholders. During the course of our project, we developed materials to improve resident access to ACP and to ensure bereavement support for families. Results also suggest the pamphlets offer important information that improve resident and family comfort with engaging in ACP conversations.





